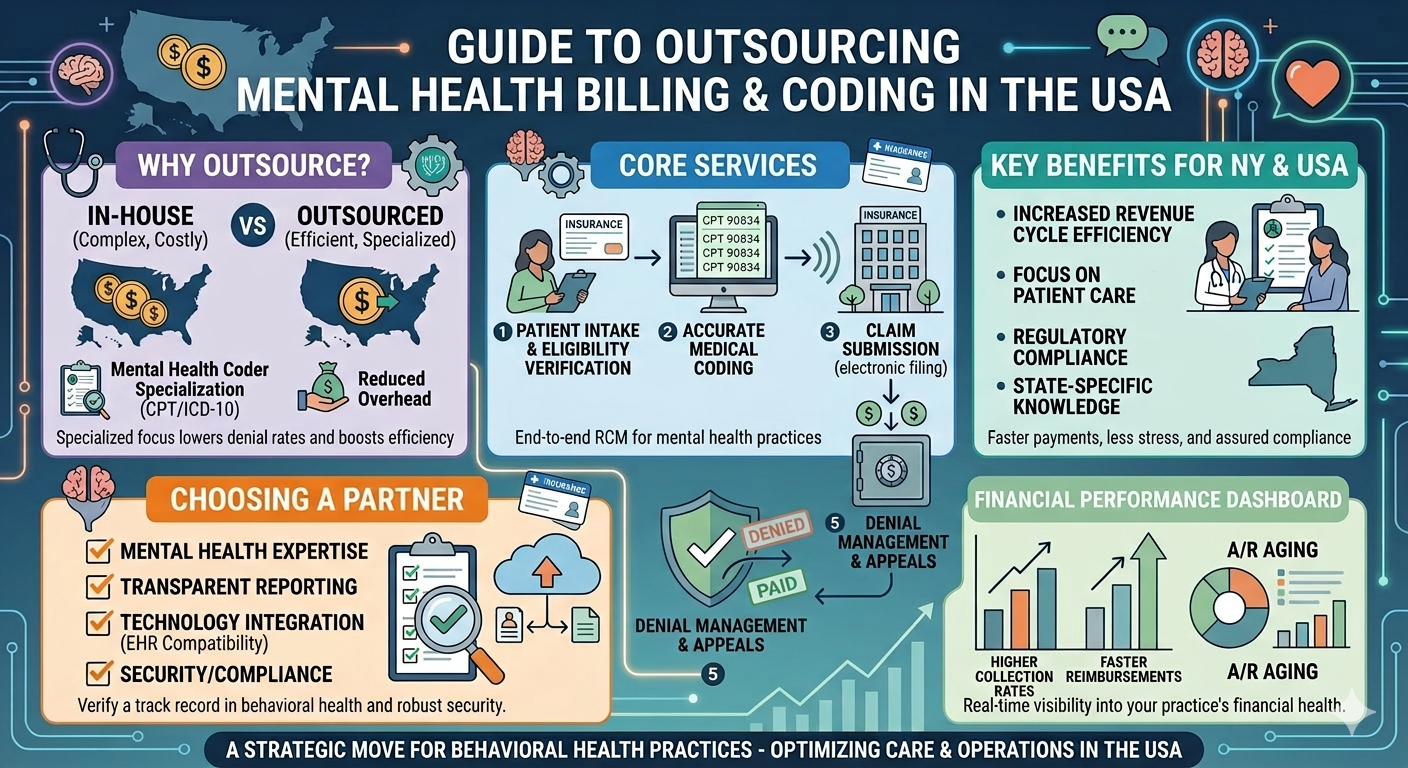
Behavioral health practices across the USA face unique billing complexities that go far beyond standard medical claims. From evolving payer rules to strict documentation requirements, even small errors can lead to denials, delayed reimbursements, or compliance risks. That’s why adopting a reliable healthcare behavioral health billing solution has become essential for sustainable growth and financial stability.
This guide explores how modern billing solutions work, why they matter, and how providers can choose the right approach to optimize revenue without compromising patient care.
Introduction
Behavioral health billing is not just about submitting claims—it’s about navigating a highly regulated and detail-driven system. Providers often deal with therapy sessions, substance use disorder treatments, telehealth services, and varying payer guidelines, all of which demand precision.
Here’s why the right solution matters:
-
Improves claim accuracy and reduces denials
-
Ensures compliance with changing regulations
-
Speeds up reimbursement cycles
-
Enhances overall revenue cycle performance
-
Allows providers to focus more on patient care
What is a Healthcare Behavioral Health Billing Solution?
A healthcare behavioral health billing solution is a structured system that manages coding, claim submission, denial handling, and payment posting specifically for behavioral and mental health services.
Unlike general billing systems, it is tailored for:
-
Psychiatry and psychology services
-
Substance abuse disorder treatments
-
Counseling and therapy sessions
-
Telehealth and virtual care
It integrates workflows that support medical billing behavioral health requirements, ensuring that every service is properly documented, coded, and reimbursed.
Key Components of Behavioral Health Billing Solutions
Accurate Coding and Documentation
Behavioral health services rely heavily on precise CPT and ICD coding. Even minor documentation gaps can trigger denials. A robust behavioral health billing service ensures:
-
Proper use of therapy and psychiatric codes
-
Documentation alignment with payer expectations
-
Reduced audit risks
Claims Management
Efficient claim submission is at the core of any behavioral health billing agency. This includes:
-
Clean claim submission on the first attempt
-
Electronic claim tracking
-
Faster processing timelines
Denial Management
Denials are common in behavioral health billing due to authorization issues or coding errors. A professional behavioral health billing company focuses on:
-
Identifying root causes of denials
-
Timely resubmissions
-
Preventing recurring errors
Compliance and Regulations
Regulatory requirements differ by state and payer. Whether it’s behavioral health billing maine or a behavioral health billing company in california, compliance must be localized and updated regularly.
Why Providers Choose to Outsource Behavioral Health Billing
Managing billing in-house can be overwhelming, especially for growing practices. This is why many providers choose to outsource behavioral health billing services.
Reduced Administrative Burden
Outsourcing eliminates the need for in-house billing teams, reducing operational stress and costs.
Access to Expertise
A behavioral health billing services company brings specialized knowledge in coding, payer policies, and compliance.
Improved Revenue Performance
The best outsource behavioral health billing and coding services focus on maximizing reimbursements while minimizing delays.
Scalability
As practices grow, outsourcing behavioral health billing and coding allows seamless expansion without increasing internal workload.
Regional Expertise Matters in Billing
Behavioral health billing requirements can vary significantly across states. Choosing a provider with regional expertise can make a major difference.
-
A behavioral health billing services company florida understands Medicaid and payer-specific nuances in the state
-
The best behavioral health billing company new york is familiar with complex insurance networks and compliance standards
-
Providers searching for behavioral health billing services near me often prioritize local expertise for better communication and faster resolution
This localized approach ensures higher claim acceptance rates and fewer compliance risks.
How to Choose the Best Behavioral Health Billing Services Company
Selecting the right partner is critical for long-term success. Here are the key factors to consider:
Industry Experience
Look for a top outsource behavioral health billing company with proven experience in mental health and substance use disorder billing.
Technology Integration
Modern behavioral health billing solutions should integrate with EHR systems for seamless workflow.
Transparency and Reporting
A reliable behavioral health billing services company provides:
-
Real-time reporting
-
Revenue insights
-
Clear communication
Customization
Every practice is different. The best behavioral health billing services company tailors its services based on:
-
Practice size
-
Specialty
-
Patient demographics
Benefits of Outsourcing Behavioral Health Billing
Outsourcing has become a strategic move for many providers aiming to optimize revenue cycle performance.
Higher Collection Rates
Experienced billing professionals ensure accurate claim submission and faster reimbursements.
Fewer Errors
With dedicated expertise, outsourcing reduces coding and documentation mistakes.
Time Savings
Providers can focus on patient care instead of administrative tasks.
Cost Efficiency
Hiring and training in-house teams can be expensive. Outsourcing provides a more cost-effective solution.
Challenges in Behavioral Health Billing
Even with the best systems, challenges persist:
Frequent Policy Changes
Insurance policies and reimbursement rules change regularly, requiring constant updates.
Complex Coding Requirements
Behavioral health coding involves multiple variables, including session duration and treatment type.
Authorization Issues
Many services require prior authorization, which can delay claims if not handled properly.
High Denial Rates
Behavioral health claims often face higher denial rates compared to other specialties.
A professional behavioral health billing company helps overcome these challenges with structured workflows and proactive management.
The Role of Technology in Modern Billing Solutions
Technology is transforming the way behavioral health billing services operate.
Automation
Automated systems reduce manual errors and improve efficiency.
Analytics
Data-driven insights help identify revenue gaps and optimize performance.
Integration
Seamless integration with practice management systems ensures smooth operations.
These advancements make healthcare behavioral health billing solution systems more reliable and scalable.
Why Behavioral & Mental Health Billing Services Are Unique
Behavioral & mental health billing services differ from traditional billing due to:
-
Time-based coding structures
-
Frequent need for detailed documentation
-
Strict compliance requirements
-
Increased focus on patient privacy
This uniqueness makes specialized billing solutions essential rather than optional.
Future Trends in Behavioral Health Billing
The future of behavioral health billing is evolving rapidly:
-
Increased adoption of telehealth billing
-
Greater focus on value-based care
-
Enhanced compliance requirements
-
Advanced AI-driven billing tools
Providers who invest in the right behavioral health billing solutions today will be better positioned for future growth.
Conclusion
A well-structured healthcare behavioral health billing solution is no longer a luxury—it is a necessity for modern practices. From improving claim accuracy to ensuring compliance and boosting revenue, the right solution can transform the financial health of any behavioral practice.
Whether you choose to outsource behavioral health billing or invest in advanced systems, the key is to partner with experts who understand the complexities of the field.
In today’s competitive landscape, organizations like 247 Medical Billing Services play a crucial role by offering comprehensive support including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These integrated solutions help providers streamline operations, reduce errors, and achieve consistent financial growth.
FAQs
What is a healthcare behavioral health billing solution?
It is a specialized system designed to manage billing processes for mental health and substance use disorder services, ensuring accurate coding, compliance, and timely reimbursements.
Why should I outsource behavioral health billing services?
Outsourcing helps reduce administrative workload, improve claim accuracy, and increase revenue by leveraging expert knowledge and advanced systems.
How do I find the best behavioral health billing services company?
Look for experience, transparency, technology integration, and proven results when selecting a billing partner.
Is behavioral health billing different from general medical billing?
Yes, it involves more complex coding, stricter documentation requirements, and higher compliance standards.
Can small practices benefit from outsourcing behavioral health billing?
Absolutely. Outsourcing provides cost-effective access to expertise and scalable solutions, making it ideal for small and growing practices.
What should I look for in a professional behavioral health billing company?
Key factors include industry expertise, strong denial management, real-time reporting, and customized solutions tailored to your practice needs.